Dr. Alona Emodi-Perman, Prof. Ilana Eli, Dr. Jawan Sleiman, and Dr. Pessia Friedman-Rubin from Tel Aviv University Maurice and Gabriela Goldschelger School of Dental Medicine published their findings in the Journal of Clinical Medicine.
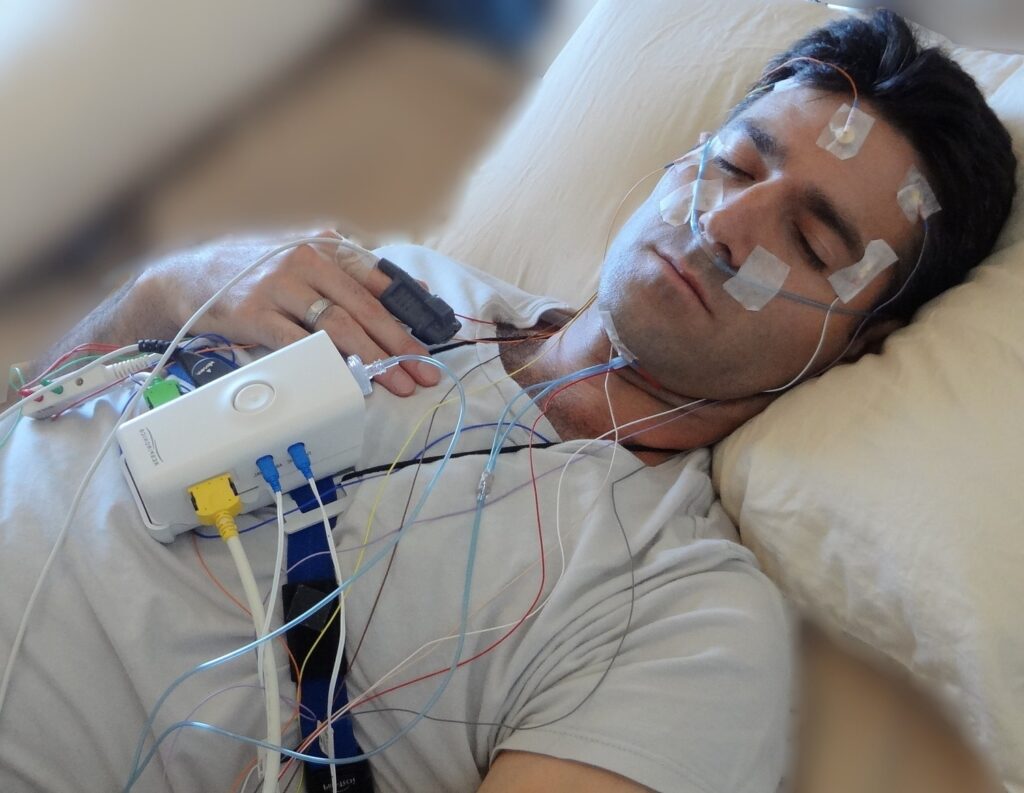
The study showed that women aged 55 and over who snore are highly likely to develop sleep apnea and that it can be lethal. The most critical aspect of this issue is that this phenomenon happens during sleep. Therefore, most women who are victims of sleep-disordered breathing are completely unaware of the disease. In addition, they are at higher risk for sleep apnea.
The study fundamentally consisted of hundreds of women. The research team studied two groups of Israeli women in particular – with ages ranging from 20 to 40 (pre-menopause), and women who are aged 55 and over (post-menopause).
The findings depicted that about 15% of the women from the older age groups are at a higher risk of sleep apnea whereas, from the younger group, only 3.5% were at risk. These percentages were based on the scale of subjects in the study. Therefore, they may vary on a larger scale.
Furthermore, the association between snoring and sleep apnea was discovered based on the results of the findings. Sleep apnea risks were only 1% among the women who do not snore. On the other hand, 11% of the women who snore were at risk. This marks the difference as quite prominent.
According to Professor Eli, sleep breathing disorders tend to vary from minor snoring to the most serious and fatal disorder, sleep apnea.
Regardless of such a subtle origin, sleep apnea causes a reduction in blood oxygen concentration and can be a lethal condition. In addition, if sleep apnea is not detected and treated promptly, it can lead to the development of several systemic disorders, including cardiovascular disease, stroke, and hypertension.
Prof. Eli further states that the difficulties for proper diagnosis are mainly due to unawareness and under-reporting. Aforementioned, this condition is experienced while sleeping and there is hardly any recollection of it after waking up.
However, upon waking up, the women reported headaches, masticatory muscle soreness, fatigue, and insomnia to their doctors. Since there is no direct report of sleep apnea, the physician needs to ask the right questions and determine whether it is sleep apnea or not.
Following these findings, the research team addresses the doctors, particularly the ones specializing in the orofacial region. All symptoms even the ones giving the tiniest hint of sleep apnea should be taken into account. Moreover, asking odd questions, if the patient snores, or experiences headaches or neck discomfort while waking up should not be neglected.
Sleep apnea is almost invisible until it takes its toll. Therefore, the physician must pay extra attention to identifying the symptoms. By making use of the best practice, women who are under the radar due to unawareness and under-reporting can be provided with life-saving care.